
I’ve been asked to run an Airway Workshop for rural doctors at the annual RDASA Masterclass conference to be held in Adelaide 2015. Airway management is an essential skill for the rural clinician and one with which I am slightly obsessed…
“Without an airway, you’ve got nothing!“
This is also an area of expertise that can appear daunting to the rural clinician who doesn’t have the opportunity to maintain airway skills in theatre, or for those who are, by very nature of infrequency of airway catastrophe, so-called ‘occasional intubators‘.
Yet airway management is paramount to patient safety and where attention to “doing the basics well” can achieve real gains. Many of us learn airway management on the usual alphabet courses – APLS, EMST, RESP/REST, ELS. Yet practicing techniques on a mannikin is a world apart from the critically ill airway – these are the times when the rural clinician needs to be able to pull out the stops and deliver…more so because there is usually no immediate backup at 3am in the isolated rural hospital.
Training for difficulty is something we introduced at the #smaccUS airway workshop – I was privileged enough to run the ‘suction assisted laryngoscopy & airway decontamination’ (SALAD) sim using a mannikin designed by mad-scientist Dr Jim DuCanto from Milwaukee, US. This realistic mannikin allowed soiling of the airway from a slight trickle of vomit…to a veritable poltergeist-like geyser. Even seasoned intubators broke into a sweat when this baby was cranked up…
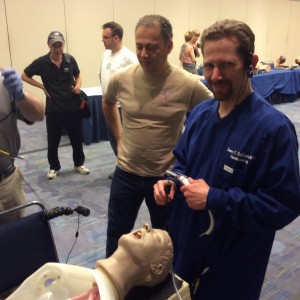

Airway Thrills – Session Outline
With only a two hour session to impart some skills and make the session rewarding, I’ve decided to forego the usual didactic training and instead run some interactive sim scenarios. Sadly critical illness does not respect geography, so the ‘Airway Thrills” session will immerse attendees in some gnarly situations which will require skills such as teamwork, airway planning and some of the finesse gleaned from FOAMed circles and not taught on the usual alphabet courses.
Basics skills such as insertion of oro- and nasopharyngeal airways will be taken for granted, as will bag-mask ventilation and the technique of endotracheal intubation. We will have a short time to recap some hands-on skills using task trainers, with choices determined by individuals’ preferences and past experience. Specific skills refreshment will include
- two hand BMV technique and use of PEEP
- emergency surgical airway technique
- DL vs VL hands-on refresher
- next generation supraglottic devices (LMAs) and their use as a conduit for blind/FO intubation
..and then we will move into the sim sessions – aka “Nightmare on Airway Street”

Sim sessions can be scary for clinicians – especially when pitched to test skills with difficult scenarios. Yet our patients require that we are up-to-date and competent to deal with emergency presentations.
One of my bugbears is that many mandatory courses are devoid of FOAMed content and aimed at specific craft groups only. The rural resus team is comprised of doctors and nurses; in Country Health SA, the doctors are usually private practitioners engaged on a fee-for-service model, whilst the nursing staff are salaried. As such, I am unaware of any routine training as a team – instead the CHSALHN nursing staff do their mandated training and the doctors do theirs, they rarely train together. Neither is audit of high-acuity (typically retrieval) cases embedded in the culture of rural hospitals in SA – something I am anxious to change.
“Please…not another mandatory CPR refresher“
My colleague Andy Buck (of ETMcourse) emphasises the importance of ‘flash teams’ – the fact that resus teams are made up of individuals who have not trained together and yet are required to perform potentially complicated tasks under situations of high stress, without making mistakes. In situ simulation using own equipment, staff and with realistic scenarios such as sepsis, chest pain, paediatrics etc are worthwhile, not the usual mandatory CPR-AED sessions.
I won’t give away the scenarios in full here; suffice it to say that attendees will get to meet each of the following patients and be required to manage them as a rural resus team using the standard equipment in CHSA hospitals…
Mr Creosote – 140kg gentleman in ED with community-acquired pneumonia
PMHx includes COPD, OSA, HT, T2DM – RR 30 HR 100 BP 100 SpO2 87% 15l NRB
Ms G Gee – 20 yo who has fallen from horse & been trampled
Responds to pain only- RR 26 HR 10o BP 100 SpO2 80% 15l NRB
Mad Mike – has been off his psych meds & using methamphetamine
An involuntary patient under treatment order who is currently destroying your ED & will need emergent sedation “Code Black”
Resources
Hopefully these scenarios and the airway challenges therein will generate some incentive for doctors to go back to their own institutions and embrace in situ sim training using their own kit, staff and know-how. If that translates to more confidence dealing with airway management and, better still, improved outcomes, then all the better!
On that latter note of knowledge, FOAMed can help narrow the knowledge translation gap. Here are some recommended resources for the “Airway Thrills” session…
- Stylets & Bougies video
- Laryngeal Masks update video
- Difficult Airway Kit on a Budget video
- Rural Resus Room Management video
- Being Expert Enough (talk for “Critically Ill Airway” course) slideshow
- BMVs & Oxygen Delivery (from Monash Anaesthesia’s Nicholas Chrimes)
- Why you should always add a PEEP valve to your BMV (from George Kovacs at AIME)
- Ramping the Obese & Delayed Sequence Intubation – essential reading from EDexam.com.au
- Weingart & Levitan’s paper “Pre-oxygenation & Prevention of Desaturation in the Emergency Department” PDF – read it, implement it, practice it
- Airway Plan PDF
- RSI Kit Dump PDF
- RSI Checklist PDF
- Real Airway Doctors Should Use Checklists – Debate video
- Oxylog 3000 Basics video from Jo Deverill
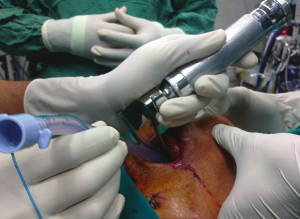
- Emergency Surgical Airway “scalpel-finger-tube” and relevant ESA mindset
- The Laryngeal Handshake
- Consensus Statement for Management of the Acutely Agitated Patient in a Remote Location PDF
- Surviving Sedation Guidelines PDF
- Rural Emergency Responder Network crisis Action Cards (download PDF here)
- Theatre & ED Crisis Checklists PDF
- Human Factors – The Elaine Bromiley Case & Teamwork from Simpact (webpage, blog, videos)
- Interhospital Patient Packaging from GSA-HEMS
- Essentials of RSI (prehospital airway expertise from GSA-HEMS)
- How We Train is How We Fight – video showing good use of sim by an expert retrieval service
My recent paper in Critical Care Horizons discusses some relevant RSI modifications for the critically unwell which ay be of interest to rural doctors – read it at Critical Care Horizons or download as a PDF
Enjoy!

Great to see this Tim. Wish you could bring it to WA too!
If you are keen I am happy to try and make it happen
C