Many people are eagerly awaiting the release of the new Difficult Airway Society UK (DAS UK) guidelines, in the wake of their recent Annual Scientific Meeting.
Some recommendations are available HERE and include :
- acceptance of gentle mask ventilation during RSI
- use of videolaryngoscopy as an option in initial intubation plan
- apnoeic diffusion oxygenation
- didactic technique and training for emergency surgical airway
One other recommendation caught my eye – namely to use second generation LMAs
Now the Classic LMA (cLMA) was the brainchild of Archie Brain; it is a wonderful device and has been in commercial use since 1987. It is easy to use and affords the ability to ventilate – although does not protect the airway. Some critics would argue that the LMA has deskilled a generation of anaesthetists, who may use the cLMA for routine cases rather than bag-mask or intubate. I disagree – it is just another tool in the armamentarium.
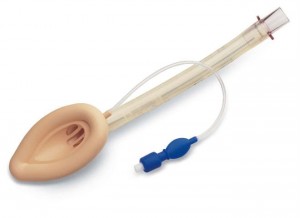
However I made a decision a few years ago to switch to the Supreme LMA – a lovely second generation LMA that is a step up form the ‘initial’ second generation LMA (the ProSeal). The Supreme combines an integral bite block with a gastric drainage channel in the tip, unlike the ProSeal.
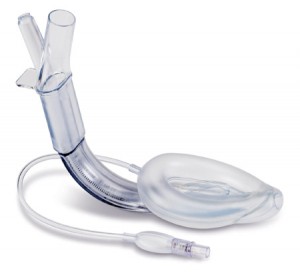
Note gastric drainage channel at tip of the LMA bowl (R)
But there is a problem – once in place, it is almost impossible to pass an ETT tube through the Supreme.
Many people will be familiar with the Intubating LMA (iLMA) – the brand most use ins the FastTrach. It’s not a bad device – it allows blind intubation rates of up to 90%, using the LMA as a rescue ventilation device and then as conduit for an ETT.

The large handle on the device is designed to facilitate manoevuring of the iLMA in the oropharynx, ideally allowing the bowl of the LMA to align with the glottic opening and hence allow blind passage of an ETT. There is a great paper from the originator of these maneouvres, Chandy Verghese. A description is available HERE – anyone using the FastTrach should be able to perform the “Chandy Manouevre(s)”
I like the FastTrach – it is a good ‘go to’ device for rural and remote doctors as allows both rescue ventilation and possible intubation – no pissing around with fancy fibreoptics or calling for help – none is available in the bush! However there are some problems – it’s expensive and it doesn’t have a gastric drainage channel. Furthermore, one can get into a world of hurt if attempting to remove the iLMA over the ETT per instructions. This might include stripping off the pilot cuff of the ETT or ‘losing the airway’…one should read the infamous ‘exploding scrotum‘ case for a masterclass in airway catastrophe.
So problems with the FastTrach are not uncommon in inexperienced hands – precisely the time when you least want to have an additional problem after failed intubation. My advice? Once in, leave both iLMA and ETT in situ until the patient is either awake or you are somewhere with backup!
Furthermore, the FastTrach has a somewhat hyperacute angle, meaning that even if you have a basic fibreoptic device (such as a malleable FO stylet), this cannot be used to turn blind intubation into fibreoptic intubation via the iLMA conduit.
What we need is a device combining the benefits of a second generation LMA (eg Supreme) with an intubating LMA. Enter the second generation iLMA, the AirQ-II
I first heard of these in 2011 from James duCanto in the States. They’ve also had some coverage from Scott Weingart over at EM-Crit in the past. It’s basically a second generation iLMA which is :
- cheap
- useful as a rescue ventilation device ie 2nd generation LMA
- able to be used as an intubating LMA for blind intubation
- less acute curvature of the tube will allow passage of both flexible and malleable stylet fibreoptics, for visual intubation
- integral bite block and gastric drainage channel
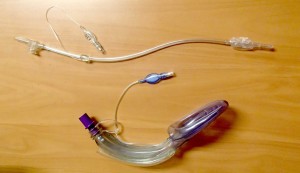
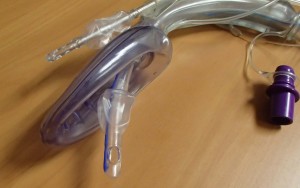
I’ve replaced the FastTrachs with Air-Q IIs in both my RERN prehospital pack and also on our hospital difficult airway trolley. Indeed, for the finance-limited environment of a small rural hospital, the combination of the AIrQ-II along with a fibreoptic device such as a Levitan FPS scope offers a fairly robust option for difficult intubation – drop in an AirQ-II, then wither blindly intubate or use the malleable fibreoptic stylet to pass the tube under direct vision. Then leave the ETT-LMA in site and pop down an orogastric (difficult to do with the FastTrach). James DuCanto writes well on this with a simple guide and Weingart explains how to mould a malleable stylet to conform to the AirQ anatomy.
If you don’t need an intubating LMA, then follow the guidance of DAS2015 and go with a second generation supraglottic device – like the Supreme.
But if you want to allow maximum flexibility including integral intubating-LMA capability, it’s hard to beat the Cook Gas AirQ-II – especially of trying to put together an affordable yet robust difficult airway kit for rural/remote.
DISCLAIMER – I HAVE NO FINANCIAL TIES OR INTERESTS TO THE DEVICES DISCUSSED
Hello Tim, Im Mercury Medical’s distributor in Costa Rica and have found that most specialists arent interested in better technology but rather in maintaining the status quo perhaps because of their personal interests which would be very linked to the benefits of supporting LMA which would include payments and trips to congresses etc such as described by the following article.
http://www.npr.org/blogs/health/2014/11/26/366618323/patient-safety-journal-finds-violations-tightens-standards-after-scandal
Its come to the point where the AirQ has been used but has never been allowed to be an intubating device as that “throne” is reserved for the Fastrach despite it being 4 times more expensive.
Any comments or articles related to that mention is appreciated. Thank you and best regards.
Pingback: DAS 2015: Ditch the FastTrach? - KI Doc