Like most clinicians, my time spent in anaesthesia drilled me in the importance of performing routine pre-anaesthetic machine checks, of keeping the workspace tidy and paying meticulous attention to detail. ‘
These lessons translate well into other areas of practice – at the start of every on call period in emergency, I check the resus trolley and store boxes to ensure we have the right kit available. In recent times I’ve begun to think more and more about resus room ‘feng shui’ – the concept of making sure that the components of the room are ordered correctly, eg :
- resus & airway trolley on the intubator’s right side so as not to impede visual axis during intubation
- all monitoring/O2/suction cables & tubes running from single point, allowing almost complete 360 degree access
- orientation of bed so that clinicians can see monitors, clocks, whiteboard, equipment etc
- colour-coding of equipment so as to group kit together for those unfamiliar with set up or in a crisis
- clear signage to essentials such as defib, difficult airway trolley, paediatric kit etc
Working with MedSTAR retrieval builds on this and I get to indulge by obsessive compulsive disorder (it’s called OCD, but aficionados know that it should be called CDO – you…have…to get…letters…in…right order).
Every day starts off with a full kit check (using a challenge-response checklist), then kit tagged and labelled – anything with a broken seal gets a full re-check. Packs are colour coded to aid recall in a crisis (it’s easy to ask a firefighter to get the ‘small red pack sitting in the big blue pack’ rather than tell ’em to get the arterial line kit). MedSTAR uses an RSI kit dump plastic bag that doubles as a clinical waste repository, with an integral challenge-response checklist.
One of the two-person team (typically doctor-nurse or doctor-paramedic) carries a drug pouch with Schedule 8 drugs (fentanyl, ketamine etc). The team always carry pagers, GRN radio and an iPhone (the latter contains checklists for daily kit checks, contact numbers and SOPs).
In recent times an iPad Mini has become available as an option – although no good as a communication device (unless use FaceTime or Skype!), it is easier to use for performing checklists and reading SOP PDFs. It also allows for addition of useful clinical apps such as Matt & Mike’s excellent Bedside Ultrasound iBook and pre-loading with FOAMed content (podcasts, vodcasts etc). The problem though had been where to carry it – the iPad mini JUST fits into a pocket on the flight suit. Stuffing it into a pack means you’re never likely to use it – it’ll be stored in the back of ambulance, tied down in flight or otherwise inaccessible.

Despite initial scepticism, I have been using Twitter for the past 18 months to connect with #FOAMed enthusiasts – it’s a great tool for signposting and sharing information from likeminded people around the world, some of whom I have met, some not. Retrieval clinician Natasha Burley (@skimightythings) put out a tweet of the GridIt system in use with Careflight, Queensland a few weeks ago…a sensible idea so good that I had to try it!
So for the past few shifts I have been experimenting with the GridIt system. This is basically a neoprene sleeve and folder for phones, phablets, tablets and PCs, with a series of interlocking bands forming a grid into which chargers, connectors etc can be placed. It’s marketed to power users who carry lots of kit. I find it quite useful for giving presentations as I can make sure I’ve got my projector controller, VGA/HDMI adaptors, power cords, audio cable and other sundries available when giving a talk off home ground.

DISCLAIMER – I HAVE NO PROPRIETARY INTEREST IN GRID-IT NOR IS THE DEVICE ENDORSED BY MedSTAR RETRIEVAL SERVICE. THIS REVIEW IS MY OWN OPINION.
The question is as to whether it would ‘value add’ for the retrieval setting. I managed to snaffle an iPad Mini GridIt pouch (had to hunt for the MedSTAR red version on eBay) and experiment with it during a typical shift.

I was pleasantly surprised. The neoprene pouch is easy to carry and non-slip despite the recent hot weather (temperatures in the 30s). The iPad Mini fits snugly in the pouch and is further protected by a fold over sleeve. Having the iPad Mini available at all times (rather like the President of the United States ‘football’ of nuclear access codes) meant that I was more inclined to actually USE the device for kit checks and SOPs, as well as afford the potential for mini-tutes on ultrasound and listening to podcasts from my FOAMed mates (eagerly awaiting Mark Wilson & co with neuro edition of RAGE podcast). Listening to content or refreshing knowledge is always possible on the outward leg of a mission, whether by road, rotary or fixed wing.

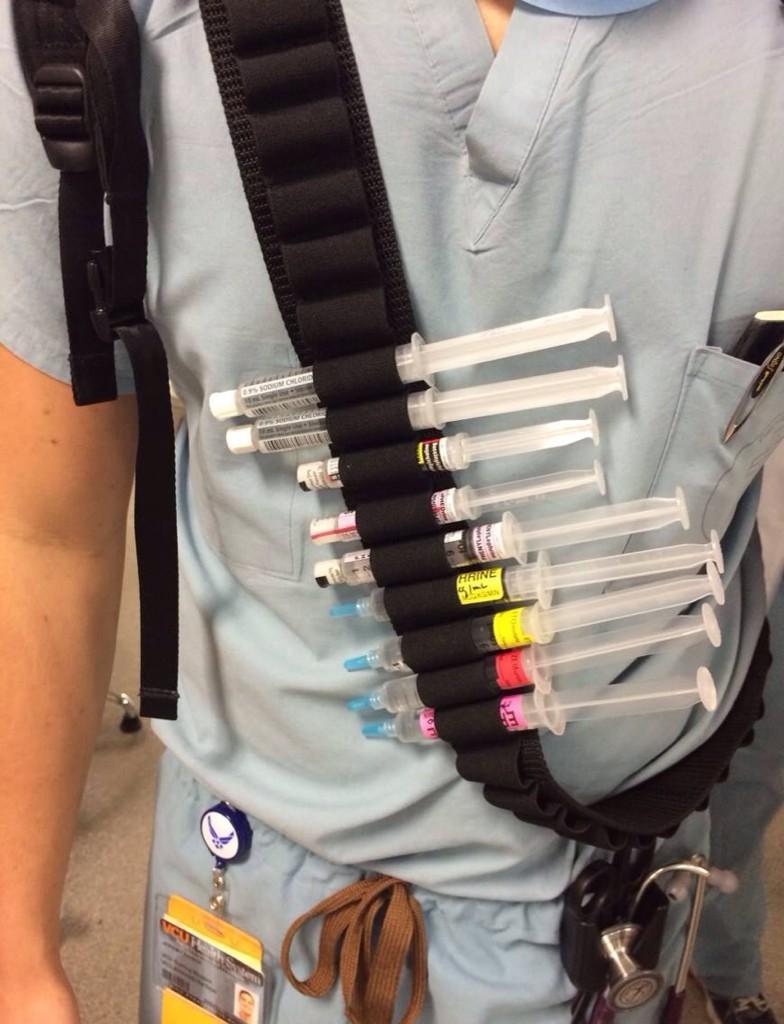
We carry our S8s on our person already, but the syringes and caps are kept in our kit, making it impossible to draw up drugs en route unless remember to get the large major drug/IV pack out before travel. By keeping a few syringes, saline and red caps plus vial access cannulae in the pouch, I found that could mix up basics (ketamine, fentanyl) at anytime using the kit on my person. Once pre-drawn, syringes were kept protected by the neoprene sleeve and readily available.
I did wonder how we would go in transit WITH a patient, especially in the crowded space of a helicopter. The photos probably don’t do it justice (lots of vibration!) but I found I could secure the GridIt system to the stretcher using the velcro cuffs – or just stuff the darn thing into a pocket if I was worried.
Depending on the aircraft and configuration with stretcher, I found could secure to either the side of the stretcher so that iPad and drugs were within easy reach (basically between legs if sitting side on to stretcher)…or secure to the head end where we already stash bag-valve-mask in a pouch.
The ability to reverse the neoprene sleeve and loop around the stretcher rail then secure with velcro worked well – but for added security one could easily add a carabiner.



We already have a system of securing pre-drawn syringes (for bolus dosing) on a hoop system on our ventilator. Many missions don’t require a ventilator, just standard monitoring, so the options have usually been to stuff syringes into a pocket on flight suit.
Adding an iPad to the mix means pockets get full or tend to either stash in a pack bag (inaccessible) or just leave the thing behind… a shame as having an iPad available could value add to missions, I feel.
Combining the iPad Mini and syringes in one system seemed to work well. I am interested in other options available out there!
And what else should we put on the ipad Mini?
The next question will be which apps and FOAMed content should be included on a tablet. MedSTAR has it’s own proprietary app for checklists and SOPs. My preference would be to add :
- useful apps for clinical conditions including neonatal, paeds, adults calculators, pharmacy support, emergency medicine resources, burns calculators etc
- links to FOAMed resources online such as LITFL, EMRAP, RESUS.ME, PREHOSPITALMED.COM etc etc or even the prehopsitalresearch forum in Australia
- links to websites of other retrieval services with free & open access content, such as SYDNEYHEMS.COM, UK-HEMS, AUCKLAND HEMS, EMRS etc
- iBook resources such as Bedside Ultrasound from those madmen & all-round nice guys Matt Dawson & Mike Mallin, or the excellent manual from ATACC (iTunes version here, PDF here)
- Podcasts from RAGE, EMCRIT, SMACC etc
- Vodcasts such as the smaccFEED from SMACC (intensivecarenetwork,com or vimeo.com/smacc)
- Sim scenarios such as those available in the shareable online global community via iSimulate
[ I am a big fan of the UK HEMS SOPs available online – http://www.uk-hems.co.uk/ukhemssops.html and the Sydney HEMS clinical governance and sim resources in particular – http://sydneyHEMS.com ]
Who knows? Perhaps in the future my mate Mark Wilson’s GoodSAMapp could be added to not just individual clinicians smartphones, but also to institutional devices – as it allows tracking of location and ‘push’ alerts integrated with comms CAD; potentially very useful in a MAJAX situation
Hey! If you are a Paramedic, Nurse, Doctor or Registered First Aider who can hold open an airway or do BLS, please take time to register with GoodSAMapp for Android or iOS. It’s FREE

Hi tim i am in remote medical care in vic and would like to see some more infomation or pictures of MedSTAR SA equipment
many thanks
mitch
As ever….totally tip top Tim. Man you’re awesome……I especially love your selfie in the helo with a sort of “ooh er missus” face. I will endevor to replicate this during my week in Toowoomba! All the best Tash