So as a pre-smaccGOLD prelude, I was able to join the Levitan Airway course held in Sydney at the Royal North Shore simulation lab run by John Vassilliadis and team. I’ve been to this sim centre before, for both the Effective Management of Anaesthetic Crises course and as adjunct to the Rural Doctors NSW conference. For those who haven’t, it’s a top notch facility on the North Shore.
The RNSH Team have run four Levitan courses so far, with more planned. Levitan also runs these courses in the States.
Background
Scott Weingart was right – Rich Levitan is an engaging speaker and manages to convey important airway messages in a mix of didactic lectures, group discussions and practical hands on. For those who don’t know, he’s the author of the ‘Airway Cam‘ book
I’d read Levitan’s book before, and to be honest despite being engaged in an anaesthetic training programme at the time, it wasn’t until reading this book that the subtleties of intubation ‘gelled’ for me.
More than anything, I was humbled to learn that Levitan now works as a rural doc himself, downsizing from the GSW-laded high-adrenaline of Philadelphia ED to a small community hospital of 25 beds in North Hampshire. More importantly, he speaks authoritatively and with great use of body language and anecdote to convey messages on airway management.
I was literally grinning from ear-to-ear after the first fourm as all the pearls from FOAMed airway management were distilled into bite-sized chunks for digestion. It was also great to see 100% hands up in response to the question “who uses NODESAT in their practice” – I’ve sat in anaesthetic “refresher” courses in the past two years, where this concept has been unheard of – by Faculty! Truly FOAMed is changing the way we practice…
Synopsis & Content
Day One was mostly lectures, with some minimal hands-on work in a nasoendoscopy session. Rather than fibreoptic, we use CMOS ‘chip on a stick’ tools (great lumens, less visual distortion) to perform nasoendoscopy either on ourselves or colleagues. Amazingly we were able to achieve this without topicalisation for the most part.
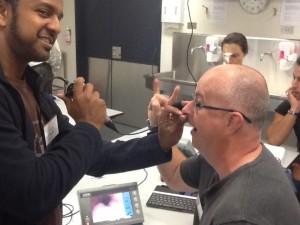
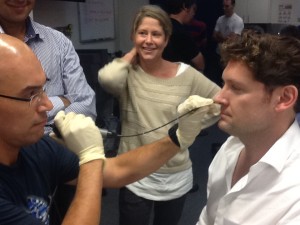

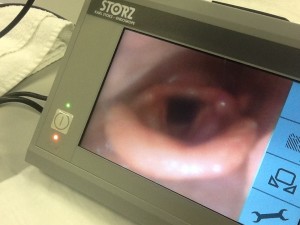
The rest of the day was spent discussing airway pearls – difficult cases, the use of DL vs VL, the mantra of OOPS (Oxygen On, Pull mandible forward, Sit patient up), using high-flow nasal cannulae to deliver oxygen as apnoeic diffusion oxygenation (NODESAT), ramping or elevation of the head the patient into an ear-to-sternum and breaking airway management down into parts – with epiglottoscopy as the key.
More than anything though, Levitan emphasised the impact of stress on performance in a crisis, the need for simplified airway crises algorithms (needless to say, The Vortex got a plus) as well as enabling team-buy in via use of checklists EVEN IN A CRISIS. There are even rumours of involving a psychologist on future courses…
RSI, parachuting and difficult airway kit
I’ve always considered RSI as a procedure needing total commitment. I’ll talk a little more about this at smaccGOLD (in the RSI checklist debate) – but essentially it’s a tightly-coupled potentially high-risk procedure. A bit like BASE jumping.
Levitan tells an anecdote of the EM & Anaes doc approach. Anaesthesia has a low tolerance of risk – whereas EM may have to embrace it. Picture the scene – an anaesthetist and an EM doc decide to go sky-diving. The anaesthetist turns to his Em colleague and says “Hey mate – you ED docs are risk takers – why don;t you use my OLD parachute? It’s not that reliable…in fact, I’ve replaced it with this brand new one which is far better“. Do you think the ED doc would take that risk? …and yet when anaesthesia turns around to ED and says “We’re getting rid of our old airway kit, do you guys want it?” the ED docs say “Hell yes!”
We really shouldn’t accept a lesser standard of care. Whether in ED, prehospital or rural. My bugbear is making sure that rural docs have the right kit and skill set to deal with the difficult airway or trauma RSI – but they need the kit.
Day Two was a day in the cadaver lab; I don’t know how he gets through customs, but Levitan imported 18 half cadavers (heads and thorax, no abdomen/pelvis or limbs) prepared in such a way that tissue elasticity is preserved and can be intubated in a variety of ways using varied kit. There really is no better way than repeated practice at laryngoscopy. This was mostly a re-hash of established routine, with emphasis on
- determination of eye dominance for intubation
- focussing on larygnoscope grip, proper positioning of self and patient to ensure maximal mechanical advantage with minimal effort
- breaking intubation down into stages – epiglottisoscopy, identification of interarytenoid notch, then maximising view of the laryngeal inlet
I am not a huge fan of stylets, preferring the bougie held in a ‘Kiwi grip’ as taught to be by Paul Baker of the ANZCA Difficult Airway SIG. But I was glad to practice the ‘straight-to-cuff’ technique of stylet, approaching laryngeal inlet from below without interruption to visual axis. Manouevres were practiced that I’ve learned through experience or FOAMed (not through formal anaesthetic teaching), such as rotating stylet right to enter trachea without impingement on the tracheal rings and my all-time favourite ‘the flip-flop’ manoeuvre as illustrated below (from GSA-HEMS, natch) for advancing ETT on bougie.
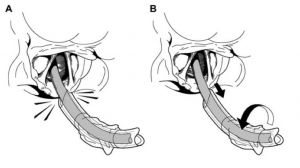
Further cadaver work included placement of a variety of LMAs, although disappointingly not the Air-Q II ‘Cook Gas’ (I’ve got these second-generation iLMAs on Kangaroo Island). I reckon the Air-Q II holds the advantages of an iLMA with bite block, gastric drainage port and allows wither blind or fibreoptic intubation – the latter with either malleable stylet or a flexible scope. There’s none of that faffing around with the FastTrach that causes problems (thin the infamous Gordon Ewings case) and has become my ‘go to’ device for maintenance of ventilation in a difficult airway.
A short session on videolaryngoscopes followed, including use of the AP-Advance, C-Mac (although disappointingly not the pocket C-Mac) KingVision and McGrath devices, as well as practice with fibreoptic and CMOS-type flexible scopes.
No airway workshop is complete without practice of a surgical airway. I’m in the rather unusual position of having done five now (one in ICU, two in ED two prehospital) – and from the initial muppet show that was my first (needle-over-wire, truly traumatic) I have reflected and refined this, now preferring a scalpel-finger/bougie-tube technique. But even on this, I was able to refine skills – Levitan teaches the ‘laryngeal handshake’ approach. I found that shutting my eyes and performing this manoeuvre allowed rapid identification of the cricothyroid membrane on all of the 18 cadaver specimens. Moreover, focussing on position (hand resting on sternum to perform scalpel incisions) was a useful pearl. Of course the surgical airway is a primarily tactile procedure, and the chance to identify and feel the CTM on 18 specimens is an opportunity rarely afforded. using the laryngeal handshake works – with 100% success in rapid (2-3 seconds) identification of the CTM on the cadavers supplied.
It was also great to see the Cric-Knife & CricKey. I’d heard about this via Minh le Cong at prehospitalmed.com and it’s been covered recently by Weingart (click here). It was lovely to get hands on with this very simple device. The integral tracheal hook that slides off immediately after CTM puncture was simplicity itself. The actual ET tube itself (CricKey) has features of a bougie – and helps give tactile feedback that operator is in the trachea not a false passage. Good to see Levitan realises the inherent benefits of a bougie over a stylet (TFIC – there was a bit of good-natured “bougie-bashing” over the course, reflecting differences in North America vs Australian practice).
Only one criticism – the actual ET tube is deformable and can potentially kink (thanks Jon Gatward for pointing this out). Unless this is fixed I may just stick with a size 6.0 ET if I ever have to do a sixth “crike”. But I am so tempted to get a couple of these – both for my CICO kit in ED/theatre, but also to demo on EMST-ATLS where the ridiculous scalpel/invert use handle technique is still considered ‘the ATLS way’
Summary
As always, an airway course like this attracted similar enthusiasts – the usual mix of intensivists, retrievalists, anaesthetists and the odd rural doctor. A chance to meet old mates and make some new friends. I think I’ve persuaded a few more people to come visit Kangaroo Island…but whether we get Levitan there is another story!
I’d recommend this course for the experienced airway operator, looking to incorporate some finesse and FOAMed goodness to his or her practice.
Any suggestions for the future? Perhaps less of the (fascinating and entertaining) didactic lectures…a bit more of the interactive case discussions or small group work. And a summary session at the end to ‘close’ the course and thanks all those who participated cleaning scopes, helping out with nasoendoscopy etc – John’s team (inc stalwarts like Toby Fogg and Jon Gatward) plus the sim centre staff and numerous airway equipment reps ensured that attendees always had hands full of airway gadgets. But these are minor criticisms.
The bottomline is that you CAN improve your practice, even by making very small changes – the so called “aggregation of marginal gains”.
If you are serious about airway management, particularly in an emergency setting and looking for some finesse to your practice or how you yourself teach others, then this course is worthwhile.