Like many other FOAMites, I am frantically putting finishing touches to my talks for smaccGOLD, the forthcoming critical care conference up in the Gold Coast.
Meanwhile the daily grind of work continues. I remain fascinated with the power of FOAMed to narrow the knowledge translation gap and bring clinical concepts with tangible benefits to the bedside for improved patient care. Along with the dissemination and discussion of ideas via FOAMed, like others I am interested in how best to practically apply knowledge learned. FOAMed has encouraged me not just to keep up with the literature relative to my field, but also to consider concepts such as clinical decision making and some of the barriers to practical implementation of knowledge.
Decision-making in a crisis is something I am passionate about. Simulation training and exploring human factors would seem to have a lot to offer to reduce clinical error, improve patient care and streamline systems – yet it is not something which is common in my arena of rural medicine.
All too often, rural clinicians (doctors, nurses and volunteer paramedics) engage in CPD updates that are either metrocentric, or infrequent. For us rural doctors, the usual round of alphabet-soup LS courses (ATLS, APLS, ALSO, REST.RESP etc) do not address human factors in clinical performance – despite the wealth of evidence of the importance in avoiding error. Similarly the rural nurses with whom I work are mandated to perform annual ALS updates and online moodle-based learning – which may tick boxes but doesn’t necessarily translate into clinical effectiveness. Moreover due to the contractual basis of rural doctors in SA (we are mostly VMOs, under fee-for-service), there is no allowance for team-training.
I must admit that I didn’t used to think about this. Instead I plodded along, accruing my usual CPD points each triennium and yet remained frustrated that that it was hard to ‘make things happen’ in a rural resus. At the same time I teach and direct on ATLS-EMST, and although this course has value in teaching ‘one safe way’ of managing trauma, it does not address teamwork and human factors which are pivotal to success.
Now that can change.
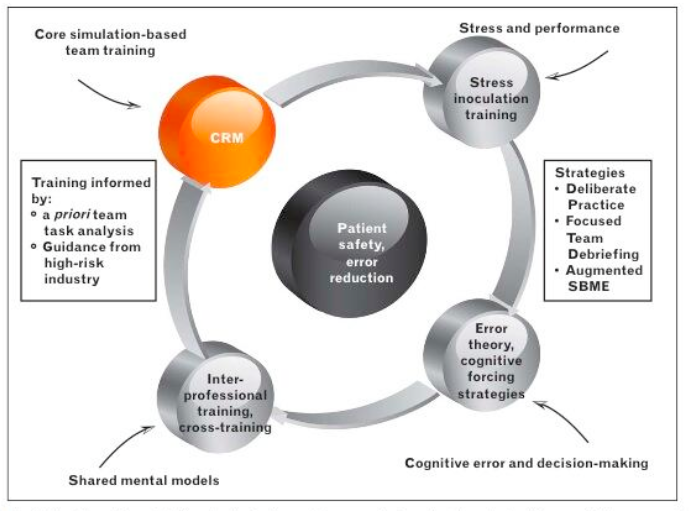
Perhaps the best way of truly understanding crisis management and patient safety is that outlined by Andrew Petronosiak, currently in Toronto. He describes a ‘Triple Threat’ approach integrating :
- mental model theory for team and task processes,
- training for stressful situations
- and metacognition & error theory
all of which lead towards a more comprehensive training paradigm than traditional methods.
Why does this matter? CRM isn’t part of the usual training we get at medical school or postgraduate training, nor on the various LS courses (EMAC & the ETMcourse being notable exceptions). If you ever had any doubts about the value of CRM, watch this powerful pecha kucha entry from @TamaraHills for the smaccGOLD conference. Then tell me you think CRM doesn’t matter…
http://vimeo.com/87966293
“Simulation – training hard in order to fight easy”
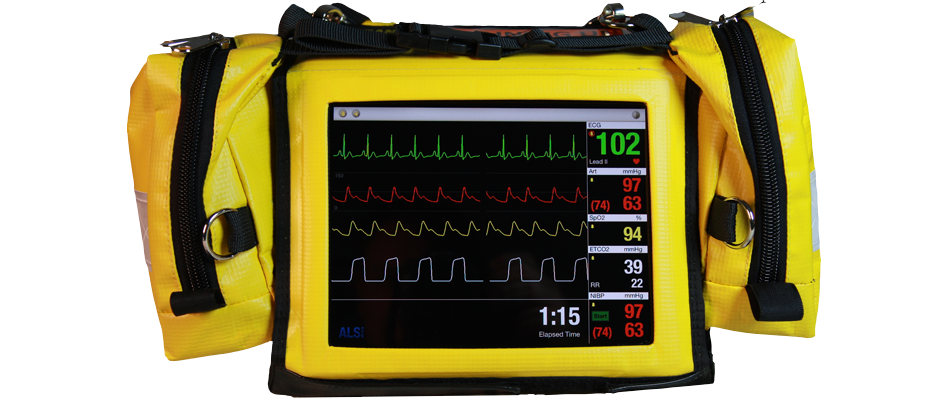
iSimulate is an affordable simulation setup, comprising two iPads and a medical equipment bag, plus assorted monitoring. It allows one iPad to be controlled by a facilitator, controlling the student iPad housed within the equipment bag in a realistic looking package. One can control HR, RR, BP, SpO2, ETCO2, temperature…throw in various rhythms, trend parameters over time, set up and store scenarios, pace, defibrillate. It even has a CTG package.
It is being used by retrieval services such as medSTAR, GSA-HEMS and Auckland HEMS. Many city hospitals use it for training. Even the Govt has got on board with sim, offering education via the NHET-Sim program. Yet the REAL power of iSimulate (or indeed any other product) is to deliver in situ training using own team, own equipment in so-called high-rep, low fidelity simulation. Jon Gatward gave an excellent talk on the concept of guerilla sim at the smacc2013 talk, which I highly recommend – especially if anyone has doubts about the value of sim training.
Of course sim forms part of the core of crisis resource management – and also opens up the door to the concept of stress inoculation, used in the military and other high-performance units – with obvious implications for emergency medicine. Listen to Weingart and Reid chat about this via the EMCrit blog…
We tried a few sim scenarios as part of the 2013 rural masterclass – mostly aimed at rural doctors who are keen on rural resus and critical care, as well as members of the RERN squad. These seemed to go down well, with scenarios including intubation of an obese, septic patient, dealing with catastrophic haemorrhage, a nightmarish CICO scenario and a perimortem C-section testing the participants.
Yet sadly uptake of simulation from the local hospital has been lacklustre – the reasons for this are not clear, but from what I can gather caveats include :
(i) sim training doesn’t work as well as traditional methods
Uh, no – plenty of evidence showing benefit to sim compared to didactic training. Gatwards’ talk and slideset takes you through that.
(ii) sim training is expensive
Uh, no – whilst many sim trainers are just CRAZY expensive (think the Laerdal models), packages such as iSimulate are relatively cheap. A sim centre costs a few million to set up and tends to be located in a tertiary hospital or medical school; running costs are around $150K per year. iSimulate is less than a twentieth of that cost and has one additional advantage…
(iii) training needs are already met by annual ALS updates
Uh, no – there’s a wealth of evidence that skills fade relatively quickly. Rather than have annual updates which ‘tick the box’, evidence shows it is far better to offer more frequent repetition of sim and preferably embed into routine. If there is a spare few minutes on shift, clinicians are far better served by running a quick sim on site, using own team and equipment than an annual session held in a sim centre or LS course, using different kit.
(iv) sessions need to be specially prepared and debriefed as part of an educational package
Well, maybe. The national NHET-Sim online training gives some structure to those who wish to facilitate sim sessions. There is no doubt that a poorly structured sim and inadequate debrief will not help learning needs. But my approach is that any sim is better than none. Even a few minutes spent conducting a simulated scenario will throw up interesting information – we’ve discovered that:
- some beds won’t fit through doors (infamously the bed from labour ward to theatre!),
- knowledge ‘taught’ cannot be applied (we found that some staff don’t know the location of difficult airway trolley or PPH kit – not a fault of individuals, but an inevitable result of traditional training)
- expectations of team members will vary (typically the romantic notion that ‘the doctor’ will fix all problems in a crisis rather than understand the limitations of loss of situational awareness, cognitive overload and all the other lessons from human factors)
Debrief is critical. We now try and avoid the Pendleton ‘shit sandwich’ – I tend to use the +/delta model now – and it was gratifying to see Andy Buck and Amit Maini use same on their excellent ETMcourse…which in itself ran lo-fi, high-rep sim as a key part of their trauma training course to highlight importance of teamwork.
(v) must train using the same kit ie: if using Phillips defib, then must use this model to train
Uh, no. One has to distinguish between a task-trained and a sim-trainer. Task trainers are fine for training with one piece of kit eg: the defib, a particualrl infusion pump etc. But this is best done in a small group or in-servce session. Sim trainers allow clinicians to do so much more – to explore complex decision-making in dynamic environments, to run and re-run scenarios with debriefing. To explore impact of human factors on performance and clinical outcomes. Since using sim, initially on an EMAC course and now more routinely in own practice, I have been amazed at how much valuable learning takes place. Far more than one gets from didactic sessions, in-services or mandatory updates.
(vi) annual updates in a sim centre or lead by tertiary hospital specialists are best
Uh, no – all too often such sessions tend to focus on the practice in those institutions. Personally I am fed up to back teeth of going to courses or listening to specialists who tell me that we must have a massive transfusion protocol (uh, we have three units of O neg then it’s on to retrieval +/- walking blood bank), call ENT and a senior anaesthetist for difficult airway (uh, no, we’re on a bloody island with rural GPAs as frontline) or to get a CT head on every PFO (uh, nearest CT scanner is 250km away on the mainland).
Moreover, one of the problems of training in a sim centre or with a ‘sim roadshow’ is that the equipment doesn’t reflect that of the local hospital. In situ training reveals local system errors and local threats – location and use of key equipment being recurrent themes.
(vii) sim sessions take too long to organise
Uh, no. Anytime, anyplace, anyone, anywhere are the maxims of high rep, lo-fi ‘guerilla’ or mobile sim. Clearly the best simulator known to humankind is the brain – and we should engage it whenever possible
For example, every shift the resus trolley is checked. Ratehr than this be a mindless rote exercise of ticking off items in their respective drawers, this ten minute exercise can be turned into a practical and more importantly beneficial training tool. Pull out a piece of equipment (like a 1mg vial of adrenaline) – then ask some questions, preferably scenario-based. “Suppose a patient came into resus this shift and was septic. How would we assess them? What equipment might we need? The MO wants to set up an inotrope infusion – want options do we have? If we only have adrenaline available, how are we going to set up an infusion? How can we determine the dose and rate? Where’s the syringe driver set? Is it compatible with the retrieval service?”
Takes perhaps 15 minutes and embeds some valuable knowledge that may be useful in a crisis.
“Guerilla Sim – Anywhere, Anytime, Anyone”
I am convinced that the best way forward to improve perfromance in rural hospitals will be to integrate sim training into the ethos of daily work. I am using ‘guerilla sim’ with this years PRCC students, so far with good results (in a crisis they have been able to set up IV fluids, apply monitoring and even begin the COAT & review approach at a relatively early stage in their career). But other than a once year visit from the mobile sim lab and the usual mandatory ALS update, such training is not embraced locally. This is a shame – with the evidence showing that ‘how you train is how you fight’, it suggests that health units that do NOT engage in regular sim training are those prepared to be mediocre, not exceptional.
I do hope that Country Health SA will consider embedding sim into country hospitals – current training tends to rely on only once a year annual updates or travel to a sim centre/course. The untapped potential of sim will be to deliver in situ training using own team and equipment as part of regular education. For a relatively cheap cost, packages like iSimulate could be used in every rural hospital. Western Australia Health does this. It’s about time SA did – but will need to come ‘top down’ from the clinical lead for rural emergency and anaesthesia, rather than individual health units choosing their own adventure.
Resources
Clinical Human Factors Group – from Martin Bromiley of ‘just a routine operation’
EDwise.edu.au – from John Vassiliaidis and colleagues, mobile and telehealth sim resources online
Guerilla Sim – talk & slideset from smacc2013
MobileSim – from Jon Gatward & Co at Royal Prince Alfred ICU
NHET-Sim – a national project to train educators and technicians to deliver sim
Simulation Training in Emergency Medicine (stem.org.au) – Jo Deverill & colleagues on Sunshine Coast
Sim & Choppers – from HEMs doc and Sim Fellow Andrew Petrosoniak
If you have any doubt about the power of sim, see how GSA-HEMS incorporate into their training “how we train is how we fight” :
See also their ‘smacc2013’ simwars entry – again, featuring use of iSimulate, checklists, team training etc


Pingback: Simulation Apps - Review - KI Doc
Pingback: Leave the Sim Lab Behind at #smaccUS | LITFL: Life in the Fast Lane Medical Blog
Pingback: What Makes a Good Conference - KI Doc