Readers of the KIdocs.org blog will be aware of my feelings re: courses for rural doctors. There are a plethora of ‘alphabet soup’ or ‘merit badge’ courses out there for entry-level as a rural registrar or doctor – ALS, APLS, ALSO, ATLS(EMST) etc.
As career progresses, we are required to maintain continuing professional development. Most of us find it easiest (and most productive) to spend a fortnight upskilling in a tertiary centre – doing emergency medicine, epidurals, elective anaesthesia or obstetrics as appropriate to our skill mix and needs. There are also courses such as REST (in SA RESP) – indeed I understand that RESP is going to become mandatory to complete every three years to maintain credentialling to work in SA rural hospitals.
I did a RESP course back in August – and whilst content was relevant for rural EM, it sets the bar pretty low. It was salutary that relevant topics such as NIPPV were ostensibly ‘covered’ – yet delegates reported inability to practically apply this modality on a real patient a few weeks later. Box ticked – but functionally useless.
An ideal course would target content for the rural proceduralist, incorporating relevant FOAMed material and allow hands-on opportunities that translate into practice. The pilot ‘rural masterclass’ was one such endeavour, there are plenty more.
I’ve just got back from the RFDS STAR course. Held in Brisbane at the Queensland Combined Emergency Services Academy (QCESA), this three day course is aimed squarely at those involved in the aeromedical environment. I am not a retrievalist, but am interested in prehospital medicine (my work occasionally requires involvement) as well as managing critical illness in the rural environment. So there are intersecting spheres of expertise making this course relevant for the rural doctor. Here’s a summary :
Course : Essential Aspects of Aeromedical Retrieval, RFDS STAR programme
The RFDS STAR program (specialised training in aeromedical retrieval) is a QLD RFDS initiative. They run two courses – “essential aspects of aeromedical retrieval” and “pre-hospital anaesthesia & airway management“.
Cost & Manual: $2600
Course cost is $2600 for the course inc meals, course manual etc. Procedural grants apply for those eligible. One also needs to factor in flights, accommodation, incidentals. NB: Whyte Island is some distance from the CBD and taxi fares are of order $50-75 each way.
The course manual is well-written, encourages reflective practice and is well-referenced. FOAMed concepts are spread throughout, along with challenging case scenarios and commentary from the authors. A few ‘holy cows’ of emergency medicine are examined and debunked – cricoid pressure, ketamine in head injury, COETT for psychiatric retrieval, permissive hypotension etc. As such it is aimed at the sharp end of prehospital care and I imagine content evolves to reflect this.
Location : QCESA Facility, Whyte Island, Brisbane QLD
This is a dedicated multiagency training centre. Not only are there conference rooms and break out rooms, but also a whole ‘play area’ covering several acres comprising gantries, industrial areas, hospital emergency room, houses, earthquake zone, shops and banks, gas station, car wrecks etc – all of which can be used to simulate training including
- fire department
- paramedics
- small rural ED
- urban search & rescue (USAR)
The course is well-catered, with functional mess room and provision of on site breakfast, lunch and dinner as well as morning/afternoon tea. 3G reception was patchy.

Accreditation : ACEM, ANZCA, CICM, ACRRM, RACGP, CASA
Australian College of Emergency Medicine – 42 points
ANZCA – 2 points per hour
College of Intensive Care Medicine – 2 points per hour
RACGP – 40 points
ACRRM – 30 points plus 10 Anaes, 6 O&G & 30 Emergency Med MOPS points
Civil Aviation Authority – 13 hours of DAME CME
Delegates : 24 per course
The course I attended had a mix of RFDS doctors and flight nurses, intensivists, anaesthetists, emergency doctors, paramedics, rural proceduralists and DAME doctors. Some of the most impressive attendees were those from existing HEMS services – in particular ICPs from the Perth Rescue chopper.


CONTENT :
Day One : 08:00-17:30
– History of aeromedical retrieval
– Aeromedical physiology theory and cases
– Choice of transport platform
– Human factors in aeromedical retrieval
– Tricks of the trade (interactive)
– Skills stations & Case studies x3 (45 mins each) : bariatric, paediatric, psychiatric
Day Two : 08:00-24:00
Morning based at RFDS base, general aviation
– Skills stations x 3 (50 mins each) : stretchers & manual handling, drugs & equipment, preparation and interfacility transfer
Transfer back to Whyte Island facility
– Real world case studies
– Becoming ‘scene savvy’ – surviving prehospital environment
– Transport of trauma patient
– Stay & Play vs Load & Go, case discussions
– International retrieval
– Primary Response Scenarios (6pm to midnight)
Day Three : 08:30-15:00
Debrief from previous Primary Response exercises
Breakout sessions on airway management (two hours) and obstetric emergencies (two hours)
Military aeromedical retrieval

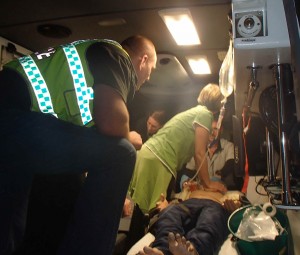
SIM SESSION DAY TWO
The primary response scenarios were challenging and fun; conducted in the ‘kill zone’ of Whyte Island, small groups rotated through nine difference scenarios…in the dark…with unexpected challenges and using first responder kit – enough for advanced airway management and haemostasis, splinting and stabilisation. Strong winds and thunderstorms added an air of realism.





Recommendations
I would recommend this course to the rural doctor with an interest in prehospital medicine. Note that the content is predominantly skewed towards aeromedical retrieval, rather than rural medicine. Interestingly three of the Faculty were rural generalists (Drs Minh le Cong, Tonia Marquardt & Shaun Parish), reinforcing my belief that rural generalism is the best ‘swiss army knife’ for prehospital and retrieval.
Even though geared towards the needs of RFDS staff, there is sufficient useful information and training in patient preparation, understanding decision-making in retrieval and tips on trauma, psychiatric retrieval, prehospital airway management and obstetric crises to be useful.
It would be worth considering the separate ‘prehospital anaesthesia’ STAR course for rural doctors with involvement in prehospital emergencies, those dealing with airways in ED or GP-anaesthetists looking for a challenge.
It certainly is at a level above the usual EMST-ALSO-RESP-APLS courses.
Criticisms
Relatively few. A credible Faculty, lots of opportunity for discussion.
I would have preferred some more emphasis on difficult airway planning and perhaps formation of small ‘flash teams’ to practice use of kit dump, RSI challenge-response checklist, difficult airway drill and extrication PRIOR to the evening exercises, in order to embed skills first within teams and to then test them under challenging circumstances. This could start from day one and perhaps allow shortening or abandonment of sessions on aeromedical physiology and history.

Pingback: RFDS STAR COURSE Review by Dr Leeuwenburg | PHARM
Pingback: ATACC Manual - Quality FOAMed - KI Doc