Why FOAMed?
Readers of the blog will be in no doubt that I am a fan of FOAMed, the revolution in medical education that has swept through the Emergency Medicine & Critical Care world. Like may others, I have got back from the SMACC2013 conference with renewed enthusiasm for cutting edge medicine and promulgating ideas amongst colleagues.
To be truthful, as a rural doctor one can feel left out at conferences – particularly those with an EM or crit care focus, as working in a rural area may be seen as lacking in rigour. Of course this is far from the truth – after all, critical illness does not respect geography. Fellow rural physicians Dr Casey Parker of BroomeDocs and Dr Minh le Cong of Prehospitalmed.com bring concepts of relevance to us rural docs.

I try to do this with KI-docs, although the focus is more about dealing with an intransigent health bureaucracy and thoughts on airway stuff than 100% hardcore critical care. The “50 Shades of Brown” section is aimed at rural doctors who are keen to embrace FOAMEd concepts relevant to resuscitation in the bush…
I hope that my talk at SMACC2013 went down OK, despite the cringeworthy jokes. You can access it HERE.
Leading on from SMACC2013, I’ve set out my manifesto for 2013-14, namely to try and achieve the following:
– to spread the FOAMed paradigm amongst rural proceduralists & help develop new FOAMed content relevant to rural doctors
– to complete the “50 shades of brown” series of “what to do when sh** hits the fan”
– ensure simple resources like RSI kit dump, checklists and awareness of NODESAT/DASH-1a are used by rural ED docs and GP-anaesthetists in Australia
– to try and badger Country Health SA into adopting an airway registry to compare rural vs metro outcomes
– similarly to incorporate more sim into training using iSimulate
– to keep plugging away on development of a rural doctor ‘masterclass’ via ACRRM
and
– to firming up rural doctors as vital members of prehospital response where gaps exist in rural Australia
I also promise to work on decreasing my scatology!
Where to from here?
I think that FOAMed has the most to offer to rural doctors – traditionally isolated by virtue of the tyranny of distance – we can now engage in high quality, relevant education and help to deliver “quality care, out there”
One of the criticisms of the current FOAMed content is that it is heavily-skewed towards resuscitation themes. I don’t think this is unreasonable – after all EM & CritCare have these at their core – so this is where most debate, controversy and innovation happens. At SMACC2013 Victoria Brazil illustrated the lack of FOAMed resources on Indigenous Health and vital public health areas such as hand-washing. I reckon we should give it time – as the FOAMed paradigm is taken up by more and more specialities (dang it, even the urologists have come on board), these topics & more will be incorporated.
Mike Cadogan’s Global Medical Education Project (GMEP) is fast becoming the repository for FOAMed resources – check it out if you have not already done so.
How to use FOAMed?
Whilst SMACC2013 was a great EM/CC conference, there were a sizeable number in the audience who had no idea of how to incorporate social media (SoMe) into their practice. Understandably they fear information overload and the hurdle of having to grapple with technology in lives that are already bursting at the seams with important things to do. Fair concerns, but can be easily overcome with perhaps a 2hr investment in time to get set up.
With that in mind, I would recommend the following
(i) Get your head around FOAMed – see http://lifeinthefastlane.com/foam/
(ii) Set yourself up with some sort of mobile device (I like the iPad) and download relevant apps – Mail and Safari will allow Email and Browsing, use GoodReader to store and read PDFs and other documents for reading later.

(iii) Selecting sites – choose wisely
You should then navigate to blogs or sites of interest and subscribe to their content via RSS. You can get this content pushed to you and collated in an easy display, rather like a constantly updated newspaper, using FlipBoard – makes browsing content from several different blogs or sites a cinch.
A common criticism of FOAMed is that is is not peer-reviewed in the same way as a journal article. That’s specious, as Richard Smith (former Editor of the BMJ) demonstrates in this article on the process of peer-review.
I reckon that peer review by putting a concept out there via FOAMed and then the ensuing debate from the worldwide community of critics is a far more robust method – good ideas will rise to the top, bad will sink.
I put out a paper last year on difficult airway equipment – the journal process took nine months – whereas FOAMed allowed me to get the concept ‘out there’ in a few minutes. I still went for the perceived kudos of getting a paper published…but in the future, I don’t know if I would bother, unless there were consequence for not doing so (plagiarism by others, loss of research funding or other penalty).
(iv) Connect in real time when it suits you
As well as getting content pushed to you via RSS/email, you may want to take the plunge and get yourself a Twitter account. To be honest I would not bother with FaceBook (it’s so last year) – I was so sceptical about Twitter, thinking it was all about Paris Hilton inanity. Instead it allows real time communication between colleagues on subjects of interest. That is powerful and highly useful for physicians – we can now connect in real time.
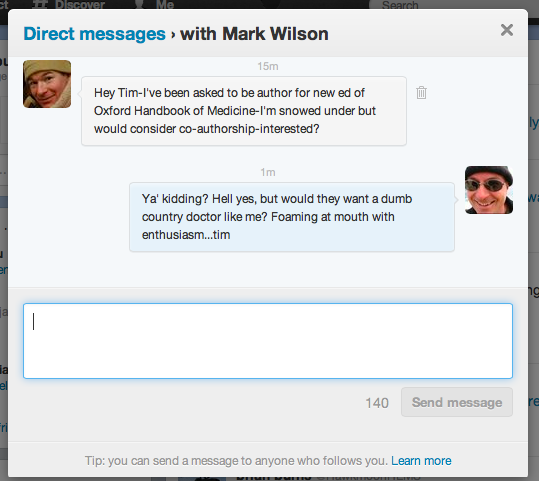
To whit, during the SMACC2013 conference I was listening to Brian Burns (@hawkMoonHEMS) talking about life-&-limb saving interventions used at GSA-HEMS. He mentioned exciting stuff like thoracotomy, lateral canthotomy, field amputation, resuscitative hysterotomy and surgical airway (three of which procedures I’ve done so far)…but did not mention decompressive procedures for extradural. If you think about it, all of these are about making holes – so why not include craniostomy? A quick tweet to my mate Mark Wilson (former rural doc, anaesthetist, London HEMS doctor and now neurosurgeon) and Mark kindly sent through to me (and a few followers) a PDF of his recent ‘How to do it’ paper on Burr holes.
That is gold – to be getting this content from a respected specialist from the other side of the world, whilst sitting in a conference in Sydney.
Similarly Minh le Cong got feedback from Karim Brohi of trauma.org on the usefulness of ROTEM/TEG in Cath Hurn’s talk on massive transfusion, after a few questions from Casey and myself on value (or not) of point-of-care INR in determining progression of ACOTS.
Summary
So Twitter is allowing clinicians with a like mind to share conversations. I am humbled to be able to talk to respected EM people like Simon Carley, Cliff Reid, Minh le Cong, Joe Lex, Mike Cadogan, Karim Brohi, Casey Parker and get a response – truly FOAMed is a meritocracy.
But to be honest, I wish that I could share these conversations with other rural doctors – there is but a handful of us involved in FOAMed – and yet the true power of FOAMed will not necessarily be in the cutting edge ‘sexy’ arenas of resuscitation – but in sharing experiences and frustrations that affect front line doctors. Traditionally operating in relative isolation, perhaps coming together once a year for an annal refresher conference, we could be so much more connected … to the benefit of our patients.
A shout out here to Gerry Considine of the Rural Flying Doc website and others like him – they are using FOAMed to cover course content in twitter study groups, to allow remote supervision (exemplified by Dr Tim Senior & Dr Michael Bonning’s forays as “supertwision”) and to effect change.
Rural doctors need to get on board and embrace the FOAMed. I am more than happy to help get you started…
Come on in and join us!
Hi Tim,
Good to meet you at SMACC. I wholeheartedly agree with you on the relevance of FOAM to rural doctors and am astonished when I meet someone who, despite having both the internet and a need for ongoing medical education has somehow, unbelievably, not managed to stumbled upon any FOAM (although i can understand how a google search on casey parker might lead certian people astray!).
Wouldn’t it be such a refreshing change for the college website to actually HAVE some useful links when you click that box? At least the ACRRM guys at SMACC were polite enough to listen to my whinging about how much their website sucked, maybe change is in the air!
cheers
glenn
Great post Tim, summed up how to get the most of FOAMed and the opportunities of Social Media for Rural Docs.
Social Media can be a great tool for Rural Docs (A point a recently made when I was applying to the Rural Generalist program in Queensland), especially addressing the issues of isolation & continuing education.
Hope to meet you one day.
Great post Tim, summed up how to get the most of FOAMed and the opportunities of Social Media for Rural Docs.
Social Media can be a great tool for Rural Docs (A point a recently made when I was applying to the Rural Generalist program in Queensland), especially addressing the issues of isolation & continuing education.
Hope to meet you in the flesh one day.