Well the “Masterclass in Rural Medicine” on Kangaroo Island is over, allowing pause for reflection. The brief was to highlight FOAMed material relevant to the rural clinician, using short interactive presentations and hands-on skills stations.

Whilst feedback was generally positive, I am always looking for ways to improve and have had some chance to think about what went well … and what didn’t. Sadly any event is a compromise between content & time with available resources & location. You can read Dr Penny Wilson’s review over at the “Nomadic GP” blog or click HERE to read Penny’s thoughts.
Formal post-course evaluations will be sent out by SAPMEA to enable claiming of CPD points and the procedural grants for those eligible.
Most of the FOAMed content discussed on KI can be found at sites such as :
Many attendees asked about the SMACC2013 videos and the infamous Elaine Bromiley video which was discussed amongst the SA GP-anaesthetists in an impromptu breakout session after the formal course.
I would encourage ANY rural doctor with an interest in the intersection of critical illness and rural medicine to attend smaccGOLD in March 2014. SMACC2013 was without a doubt the best conference I’ve ever been to. Check out registration from www.smacc.net.au – and remember, critical illness does not respect geography!
RERN members and those interested in improving resus skills attended a post-course session facilitated by Dr Hugh Grantham and Ms Chris Wilson, utilising the local hospital resus room and involving local nurses. Participants completed four challenging scenarios
- 60 yo obese patient with sepsis, requiring ramping, NIPPV, DSI, inotropic support
- 20 yo man with a fish in his oropharynx, resulting in a ‘can’t intubate, can;t oxygenate” crisis
- 50 yo tourist with complete amputation of left lower leg in a motor vehicle crash, needing control of catastrophic haemorrhage, balanced resusctiation and tranexamic acid loading
- 25 yo 38/40 pregnant female from same crash, suffering asystolic arrest and requiring perimortem C-section on the floor of resus bay…then resuscitation of the neonate.
Using iSimulate and careful debrief helped make this a worthwhile exercise. Thanks to SAAS volunteers and nursing staff who attended.

Event summary
Location : Ozone Hotel, Kingscote, Kangaroo Island, South Australia
Organised by : SAPMEA http://www.sapmea.asn.au
Coordination
Ms Nicole Thomson (SAPMEA)
Ms Chris Wilson (Flinders University)
Speakers
Dr Tim Leeuwenburg (Kangaroo Island) FOAMed & Mastery
Dr Dan Ellis (medSTAR) Critical Care in the Country
Prof Hugh Grantham (Flinders Paramedic Unit) Tips & Tricks for ED
Dr Chris Dobbins (Royal Adelaide Hospital) Trauma Tips & Tricks
Dr Yen Yung Yap (Adelaide) Obstetric Emergency Management
Dr Jamie Doube was slated to talk on ‘managing haemorrhage in austere environs’ but was mobilised as part of the AusMAT response to the post-typhoon Filipino disaster. Short videos from Cliff Reid & Scott Weingart at SMACC2013 were used as fillers.
Dan had to fly back for the SA Health awards on Friday arvo; Scott Lewis kindly stepped in to continue the skills station. Outstanding help from Mike Catchpole of RFDS QLD who registered as an attendee, but ran six repetitions of the ‘psych emergencies’ skills station for no reward. Legend.
Skills stations
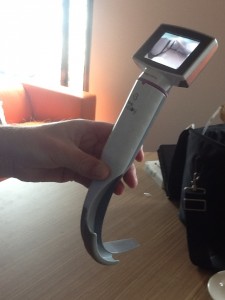
What’s new in Airway? (Tim Leeuwenburg & Jarrad Harkin)
Cardiac Conundrums (Hugh Grantham)
Trauma in the Bush (Chris Dobbins)
Agitated Delirium & Acute Psych Emergencies (Mike Catchpole)
Preparation & Packaging for Retrieval (Dan Ellis / Scott Lewis)
Paediatric Pearls (Ben Stanton)
Duration & CPD
Full day Friday, Half Day Saturday
Pre- and post-course educational activity
Eligible for ACRRM and RACGP points inc. ALS (two days)
Procedural grant funding for EM, Obs, Anaes categories (two days)
Feedback?
Informal feedback has generally been positive, although I suspect that it will take time for FOAMed and the advantages of using social media tools such as blogs, podcasts and twitter for filter out into mainstream rural medicine. Thankfully ACRRM and RACGP are on board, looking to embed this into both registrar training but also to life-long learning for established rural doctors.
The real strength of such an event is the informal ‘corridor conversations’ that happen at skills stations or in breaks. For me the most valuable time was dinner after the course and breakfast next day, where some informal networking amongst SA GP-anaesthetists highlighted common problems with equipment, training and audit that remain unaddressed within CHSALHN.
Problems?
This was the ‘cursed course’ from where I stood, with late withdrawal of key speakers, difficulty engaging the local hospital to allow on site use of OT and ED (demonstrating difficulty airway equipment, signage, resus room layout and hands-on with OxyLog etc). It was also difficulty to ensure that content remained relevant to rural doctors and was delivered by those who understand the subtleties of rural medicine. I think both Dan Ellis and Hugh Grantham spoke well to this, reflecting experience outside of the tertiary hospital environment.
Organisational matters such as travel, accommodation & location were managed by SAPMEA, as were pre- and post-course educational activities. There are considerable logistical difficulties with organising an event on Kangaroo Island, and these were dealt with.
Time wise, it is always a balance between content and available time. My preference is to offer small group, hands on sessions – but having 24 attendees, limited facilitators and a lot of content (EM-Anaes-Obs-Psych-Surgery) lead to inevitable compromise.
The future?
There was interest in running a similar event in rural SA again, probably on an annual basis. It is important not to detract from existing courses (eg: anaesthetic refresher at Lyell McEwin Hospital held every two years, RESP course required for CHSALHN credentialling every triennium).
I also feel that such a course would benefit from an extra half day, preferably involving hands-on sim training. It is a great pity that none of the KI Hospital staff attended despite being offered places; similarly it was a shame that the Hospital could not see fit to re-schedule theatre to another date to allow access to OT and ED, for benefit of both attending doctors and also the hospital staff.
My wish list for the future would be :
- an annual ‘rural masterclass’ event, sprinkled with FOAMed concepts
- rotate the location around rural Australia sites
- content to be “by rural drs for rural drs” ie: hosted and organised by rural docs
- speakers who ‘get’ the unique nature of rural medicine rather than the city specialist
- short lectures, 20-30 mins, backed up with skills sessions (small group)
- on site sim sessions involving local facilities to encourage team work
- hands on w kit such as Oxylog, difficult airway trolley, resus room management etc
- more scenarios, and (perhaps) an out of hospital RERN-SAAS exercise
- more time to interact, exchange ideas
On a local level, it was clear from many of the GP-Anaes who attended that their remains a lack of coordination in rural South Australia, with problems of kit, training and ongoing CPD shared amongst sites. I look enviously to other States (such as Queensland and WA) which have regular audit and commonality on equipment. There was a shared feeling of lack of leadership from within CHSALHN.
So – that’s my thoughts. I am interested in feedback from those who attended – either to SAPMEA (responsible for coordinating event) or to me via this blog or email.
Hi Tim,
It was a great couple of days that I found personally very useful. Some was affirmation of what I already thought but that of itself is tremendously powerful.
I also found everyone else’s stories in the “teaching session” like gaining 20 years of real experience in a few hours.
You will never get it right and you will never be happy with it because you will be always thinking you could have done it better, that is your nature and how it should be!
I didn’t sense anyone who wasn’t enjoying themselves.
Anyway, we are rural docs, if it all went well we would be suspicious.
Michael C.
Should add some specific comments.
Good mix of stations and didactic lectures, also like the way you mixed them up, though I suspect this did contribute to the musical chairs chaos on the day.
Rotate venue so everyone gets a chance to look over someone elses’ fence.
Keep it focused on rural and remote – nice to know what fancy things are done but this isn’t the focus.
The group will include a range of experience and skill levels. Balancing act between meeting the needs of those with heavy acute load while being non-threatening and digestible to those who see little acute work. This means careful selection of specialist colleagues who present.
A great weekend that was a pleasure to be involved with.
I completely agree with your “wish-list” and would love to develop the Rural Doctors Association of SA conference with very similar aims.
Watch this space…….. (Or the RDASA space. Or social media. You’ll see it! 😉 )
Yep, thanks Scott
I would favour a ‘top down’ approach to future exercises, viz
– a rural masterclass delivered under auspices of RDAA – RDASA, rotate locations and content evolve from year to year. This is do-able and should be targeted to rural docs, delivered by engaging speakers with rural u/standing.
– some specific RERN training, preferably out of hopsital, using RERN kit and involving SAAS and other agencies. Informal chat w medSTAR on this last week and offer to use their ‘dismantable’ car
– in house Hospital-based sim training for CHSALHN locations. Involve local clinicians, using own kit/staffing to foster both CRM aspects of resus AND increase application of FOAMed tips n pearls to real life clinical encounters.
Took an iSim unit up to hospital post the mass cas exercise and offered it to them for a month to train with if wanted; rationale is better for sim to be run ‘guerrilla style’ by nurses on the floor when free time rather than usual ‘once a year’ training.
Sadly rejected – nursing staff groaning under requirements of online education (often done in own time as no time to do on shift) plus usual annual ALS. Ticks the boxes, but does nothing to deliver insight into team training, CRM, checklists and cognitive aids etc.
I guess you don’t know what you don’t know. Ho hum!
Good presentation on ‘guerilla sim’ from the http://www.intensivecarenetwork.com which I will try to dig out – a concept that could and should be embrace by rural hospitals who have most to benefit from this modality of education…
…as do their patients
Tim
This is what is needed for practising emergency doctors, not the rehash of protocols that often happens ( and might be RACGP mandated) – and to be fair I think Peter Stuart in the South Australian RESP course recognises that.
I agree with Scott that similar presentations at a Rural Doctors conference would placate the masses better than a didactic lecture. THere is a compromise to be found , and we will have to work on this.
The use of social media is an eye-opener and can flash info around the place in a blink of an eye.
I am sure all who went have returned to their domicile with a spring in their step, having attended a course that recognised their skill set – that of a rural generalist!
Tim Wood
Dear Tim,
Outstanding conference
You wouldn’t believe it – my first anaesthetic this morning, couldn’t see the cords, first attempt at intubation failed, second attempt tried the bougie and couldn’t pass that, so had to use an intubating LMA to intubate.
Sailed through the operation but had ordinary sats in recovery so watched closely overnight in case he aspirated while I was fiddling about.
Pingback: Living the Island Life | Nomadic GP
Pingback: Rural Doctors Masterclass Roundup | Nomadic GP
Tim,
I wondered if you could pass on some debrief points and encouragements to the group of candidates that attended the Rural Generalist Master Class at KI on 15-16/11/13. By way of an apology, after 28 years in Air Force, I get an overwhelming compulsion to provide a Post-Activity Report.
Feel free to amend or adjust as you see fit.
Firstly, of course, I think I would probably represent the thoughts of the group in thanking the administrative and organisational staff and the coordinating and presenting staff for such a well-executed instructive and inclusive agenda. And, to whoever had The Big Idea in the first place, a special mention.
Inclusion of families was very fitting and appreciated.
I am inspired to pursue skills developments, such as obstetrics, for me, and I now have a few more points of contact, both presenters and candidates.
SAPMEA seemed to be well-positioned to assist in organisation, including pre-reading, pre-test, working on the ground, CPD admin and the post-test. I don’t know if others received the pre-test before the pre-reading list, but at the end of the day I now do now know what a DPI is.
One of the key pieces to take away was the FOAMEd structure and the availability of social media and collectives like SMACC in bringing quality education to our door (portal).
The program on the day ran very smoothly and was a credit to the coordinating and admin staff. The directing staff were not only highly esteemed, but presented the most digestible serves from their respective fields. The 20-30 minute bites with Q&A was a good sharing and learning format. There were times in the breaks and after-hours activities that I wish I could have applied my full attention to two or three discussions at once.
The candidate base was keen and brought a variety of skills and experience. It was good to have opportunities to do a fair bit of mingling and exchanging ideas. The evening social venue was conducive to this.
The highlight / climax, was the availability of the KI Hospital resus facility and nursing staff, for the directing staff to run some fairly high-fidelity (iSimulate) scenarios. I think it was a good investment for the Hospital, in terms of their own staff training and team work, as well as for the candidates.
Some may consider having the event on an island difficult for access. I didn’t mind, for myself, and I would be glad to travel there again. However, I formed the opinion that there is an expectation that future RGMC events would be spread about the state.
Having established that notion, one must consider that the location on KI also allowed you personally to maximise your effectiveness in making arrangements, with access to Hospital and the many helps that make these things happen. So a change of location is more than just the geography, but also the organisational horsepower. I suspect that if similar future events are held (annual, biannual) at a different location, then presumably someone different would be shouldering that sort of prep and coord role. I have no visibility into what the ongoing plan is, but there may be a few practices about the place that have staff levels and mix, who could bring that about.
The group this weekend was described as ‘a Cadre of GP rural generalist expertise’ and probably represented a significant minority of such like-minded people. Ongoing association is a natural progression. Various topics of interest came up, such as skills maintenance for GP Anaesthetists in the inner rural clinics, in the event that specialist anaesthetists may occupy larger proportions of theatre lists, but not be available for after-hours on-call, leaving a relatively occasional intubator to do the potentially more difficult cases, and the impact on patient safety in the rural ED. Stuff like that, but generally just having an interest group that can consult on matters of common interest and possibly even represent to Colleges or other bodies.
These are my thoughts. The main intent is to show my appreciation for a most valuable event and a hope that SA rural generalists and their patients can continue to benefit from this kind of training and collaboration.
I note talk of a class at Wirrina in August.
Thanks again to you and staff and all concerned for a most beneficial time of learning and fellowship.
Geoff Menzies (GP Anaesthetist Rural Locum)(written from Normanton QLD, 4/12/13)
Pingback: PODCAST #23 – Emergency Trauma Mx with Andy Buck @EDexam « Rural Doctors Net